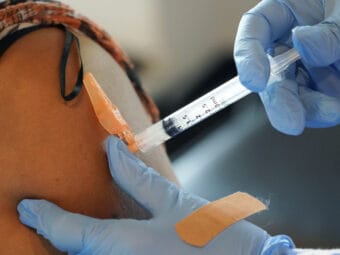
If you’ve been scrolling the Centers for Disease Control and Prevention website recently, you may have seen a paper from the Yukon-Kuskokwim Health Corporation. The paper describes how, after YKHC began using widespread rapid COVID-19 testing last fall, cases in the region dropped significantly.
COVID-19 hit the Yukon-Kuskokwim Delta hard in the fall of 2020. For weeks, the region led the nation in case rates. As the regional health care provider, the Yukon-Kuskokwim Health Corporation was traveling from community to community, testing as many people as possible for the virus.
“In a couple villages, by the time we realized there was a serious problem in the village, there were so many positive tests already,” YKHC Chief of Staff Dr. Ellen Hodges said.
That’s because it was taking an average of seven days to get the test results.
“By the time we were getting those results back, it was apparent there was a really big problem,” Hodges said.
In at least one community, an outbreak grew to infect a third of the population. The testing could not identify positive cases fast enough to contain the spread.
The tests being used at the time were polymerase chain reaction (PCR) tests. They are nasal tests that detect whether the virus’s DNA is present, and they require a laboratory. The tests are super accurate and considered the gold standard for COVID-19 tests.
YKHC had the equipment to run PCR tests in Bethel, but a national shortage of reagent, the substance needed to run the tests, prevented the health corporation from being able to use the equipment. So YKHC had to fly each test out of the region to get results. The nearest fully equipped labs were in Anchorage, but they were overwhelmed with tests from around the state. So YKHC sent many tests out of state to a private lab. All this flying of samples and so many tests meant that, on average, results took a week to get back.
“In some cases, the positive test result would come back after the patient was already out of their infectious period, which isn’t a very useful test at all,” Hodges said.
Because they needed to find a way to get results back faster to identify where outbreaks were occurring, who was infectious and how to contain the spread of the virus, YKHC began using a different test — but in a unique way. This test is called an Abbot BinaxNOW rapid test. It’s also a nasal test, but instead of testing for DNA, it tests for antigens, which are proteins from the virus. These rapid tests produce results in 15 minutes, all in one place, with no flying necessary. And they’re much cheaper than the PCR tests.
The rapid tests are extremely reliable if the result is positive. If you get a positive antigen test, you can trust that you have COVID-19. But the rapid tests are not as reliable for negative test results.
“So there’s a chance that if you test negative, you could still have COVID,” Hodges said.
But there’s a way to find out almost for sure: keep testing, a couple of days apart each time.
“If you get about three of these tests negative, that’s pretty reliable that you don’t have COVID,” Hodges said.
Called “serial testing,” this method took about the same amount of time as the PCR testing that had to be flown out — but only to be sure of a negative result. A positive result could be responded to right away. The widespread rapid testing changed the course of the pandemic in the Yukon-Kuskokwim Delta.
“We were able to get people who tested positive into isolation faster, and test their close contacts faster, and if they test positive, get them into quarantine sooner and so on, so that you could get ahead of the outbreak faster,” Hodges said.
The results were significant. Over the next month, daily cases fell by two-thirds, from 342 cases per 100,000 people during the week of Nov. 9, to 119 cases per 100,000 people during the week of Dec. 13. The overall average turnaround time for all test results also fell by nearly a third, from 6.8 days to 4.4 days.
Local leaders could learn of an outbreak and respond in real time with mitigation measures like mandated masking, screening people entering the village, cancelling large events and limiting customers in stores. Most villages in the region enforced these types of restrictions.
The results of the rapid testing were so significant that YKHC wanted to share them. The organization approached the CDC, and now Hodges is the lead author on a paper sharing the findings, along with other YKHC and Alaska colleagues.
“Our biggest hope is that other people in areas similar to ours might take this information and understand that this test can be used in their region, and it might help them reduce transmission,” Hodges said.
She emphasizes the word “might,” because it was an observational study. There were no controls used to compare one outcome against another. The results show correlation, not causation. Also, the study’s timeline occurred before the COVID-19 vaccine arrived in the region and further reduced transmission.
The paper identifies three other limitations of the study: false negatives associated with the rapid tests, that not everyone completed the series of rapid tests, variation in individuals’ responsiveness to isolation instructions, and the gap between obtaining a test result and communicating them.
YKHC continues to use both the rapid tests and the PCR tests to identify cases as COVID-19 once again surges in the region.