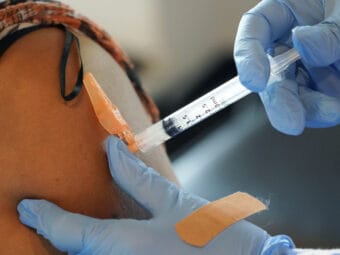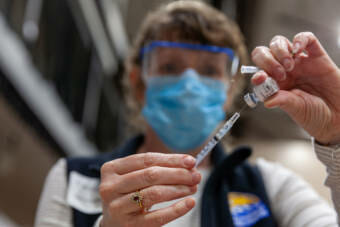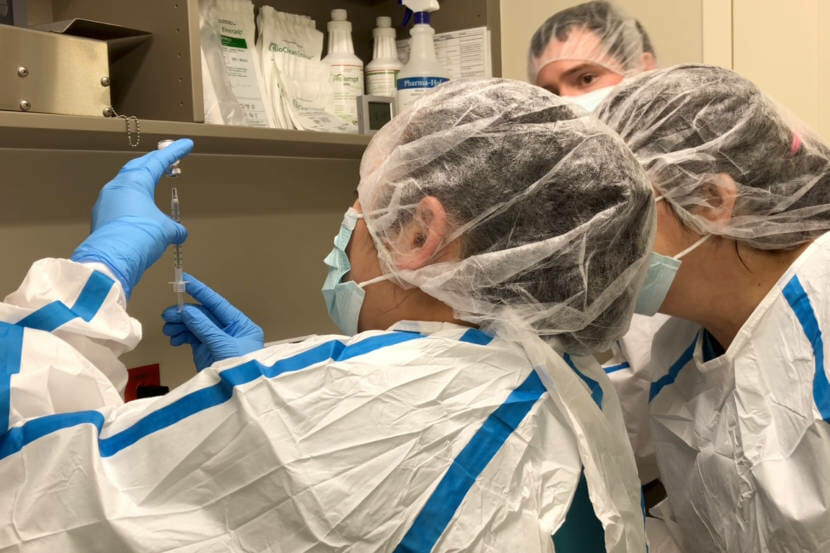
Just 22% of eligible Alaskans in the Matanuska-Susitna Borough have been vaccinated against COVID-19.
That figure is far shy of the rate experts say is required for a population to reach herd immunity — without which the virus could continue circulating, causing hospitalizations, deaths and wreaking havoc on schools and businesses.
But when Mat-Su public health officials organized a mass COVID-19 vaccination clinic Tuesday at the Alaska State Fair grounds, one-third of the 1,000 appointments went unfilled even after some providers launched a last-minute blitz to promote the event.
“We were ready to give them, and no one was there to take them,” said Dr. Mike Alter, who sent more than 100 text messages to friends urging them to sign up for shots. “I spent hours trying to get people to come to this thing.”
Alter, a longtime Mat-Su emergency physician, said he’s increasingly worried that Alaska, where some 35% of eligible residents have received at least one shot, is quickly running up against the problem of vaccine hesitancy — a problem driven by politics, misinformation and mistrust of government.
(Photo courtesy Alaska Department of Health and Social Services)
He and other Mat-Su doctors have heard from people resisting vaccines because they think the shots come from cells derived from aborted fetuses (they were used for early testing but not for production), that getting vaccinated could cancel your life insurance (it won’t) and that the shots alter your DNA (they don’t).
“I’m in the demographic that would refuse the vaccine: Conservative white male,” Alter said. “Some of my other buddies, I talked to them and heard some of their rationales, and it scares me how uninformed people are.”
COVID-19 vaccination rates vary widely across the state.
Some rural parts of Alaska, buoyed by vaccine shipments to tribal health organizations, have launched aggressive vaccination campaigns and already administered shots to more than 50% of their regions.
But providers say they’re increasingly worried about vaccine hesitancy in more politically conservative, road-system communities like the Mat-Su — an area roughly the size of West Virginia, and home to about one-seventh of Alaska’s population.
In the Kenai Peninsula Borough, 31% of eligible residents have gotten at least one shot, according to state data. That number falls to 25% in the Fairbanks North Star Borough. In Anchorage, it’s 37%.
In the Mat-Su, public health officials were already planning to pivot their vaccination strategy from mass clinics to individual providers, with whom patients have more trusting relationships. They also note that even before the fairgrounds clinic, nearly 70% of the region’s 65 and over population had received the vaccine.
But Tuesday’s unfilled appointments in the Mat-Su could foreshadow big obstacles. While appointments in many parts of the state are still quickly filling up, and federal vaccine shipments are increasing, some public health officials say they’re anxious enthusiasm will die off far short of the numbers needed for herd immunity.
Both local and national opinion polls indicate politics are a key factor in vaccine hesitancy. They suggest conservatives are particularly skeptical.
In one statewide November survey, 45% of Republicans said they wouldn’t get the vaccine. And while hesitancy rates are falling, Mat-Su doctors say they’re still encountering staunch resistance and lots of misinformation.
“I can go through and spend all day talking about why it doesn’t affect your DNA,” said Dr. Tom Quimby, another Mat-Su emergency physician who’s helped lead vaccine communication efforts in the area. “But I think if people have just decided they don’t want it, they’ll just look for the next thing to throw at you — and there are a lot of people in the wings that are willing to make up all kinds of stuff.”
The resistance is especially disheartening, Quimby added, given how successful the COVID-19 vaccines have proven to be.
“It’s just tragic to have a tool that’s effective sitting on the shelf that people don’t want to get,” he said.
Availability vs. hesitancy
In the early phases of the COVID-19 pandemic, officials said they were acutely mindful of the challenges faced in rural Alaska, where many residents can’t access ventilators or advanced medical care without getting on a plane.
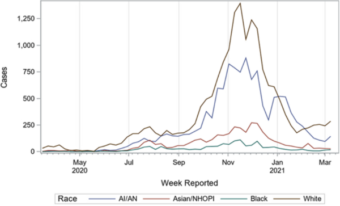
Some rural areas endured major COVID-19 outbreaks, and Alaska Native and American Indian people have accounted for double the proportion of deaths as their share of the population. But there are signs that’s changing as vaccination rates have increased, with some rural, predominantly Native areas of the state on the forefront of the country’s push toward herd immunity.
In January, the state reported more cases of COVID-19 among Alaska Natives and American Indians than among the white population. But that dynamic reversed in February, with white case rates seeing an uptick and Native cases falling as vaccination efforts kicked into gear.
In rural Western Alaska, 63% of adults in the Bering Straits region have now received at least one dose of COVID-19 vaccine, and 14 of 16 communities have vaccination rates above 50%, according to figures released this week by the tribally-run Norton Sound Health Corp.
The corporation actually turned down some of the vaccine doses it could have requested from the state this month — the first time that’s happened, said Dr. Mark Peterson, NSHC’s medical director.
“We got that 50% that were really motivated to get it, got them done, and then it wasn’t clear how many more would need it, and so you don’t want to over-order,” Peterson said.
Peterson stressed that NSHC’s efforts are far from over, given the need for much higher vaccination rates to get the region to herd immunity. And some other rural areas have far lower rates of vaccination, like the North Slope Borough, where just 28% of eligible residents have gotten at least one dose.
But Alaska officials increasingly see big challenges looming for urban and road system communities, whose vaccination rates are some of the state’s lowest.
Officials say many road system communities have simply lacked access to vaccines, and that appointments are still being booked quickly. In Fairbanks, a mass vaccination clinic Wednesday was full, with 1,200 people getting their first doses, said Dr. Mark Simon, an emergency room doctor in the Interior city.
“Our appointments have been filling up pretty well in Fairbanks, so it may just be availability,” he said. “When I see the different rates of uptake of vaccination, it just speaks to the need to try to reach out to those groups of people.”
“A very individual decision”
Over the past year, Gov. Mike Dunleavy’s administration has scrambled to get communities the resources and supplies they need to fight the pandemic, said Dr. Anne Zink, Alaska’s chief medical officer. But that dynamic is quickly shifting, she added, to one where the resources are available and the challenge is convincing people to choose to get the vaccine.
“Now, more than ever, you have a way to protect yourself as an individual, and I can’t force people to do that,” Zink said in an interview. “And it feels like a big shift. It feels like the weight of the pandemic is moving toward a very individual decision now.”
Zink and other health care experts said rural Alaska has one significant advantage in the vaccine rollout: In many areas, there’s a single system of care through tribal providers, which makes communication more straightforward.
“When you have community health aides who are really involved in vaccination and talking about effectiveness, you get communities with really high vaccine uptake,” Zink said. “But if you don’t have that same sort of engagement, that can make it much harder to really build that vaccine confidence — and I think we really see that in our urban areas.”
In retrospect, Zink said, the state also should have set up its vaccine registration system differently.
The platform was designed to connect Alaskans looking for shots with individual providers giving them out.
That was easier on clinics, who could use their own scheduling systems. But it was harder for Alaskans to navigate, and it also left the state health department without a single, unified database that it could use to communicate with residents who want to get the vaccine, Zink said.
“We were really concerned about not having enough providers,” she said. “And I think we should have done a lot more to make it easier on patients to be able to connect with a spot.”
Quimby, the Mat-Su emergency physician, said another factor in different rates of vaccine acceptance may be the immediacy of the pandemic in small rural communities, when compared to more urban areas.
“If you know everybody in town, and you know people are having to be shipped out to Anchorage because they’re sick with COVID, that’s very different than a lot of my friends on social media in the Valley who say, ‘I don’t think this COVID thing’s a big deal at all — I don’t know anybody that’s died,’” he said. “People are not scared of what they don’t see and experience firsthand.”
Quimby said he expects that as time goes by, more people will get comfortable with the vaccine. But given that political ideology appears to be such a driving force in Alaskans’ hesitancy, one of the most helpful steps in response could be a public outreach effort by conservative elected officials, he said.
“The data is telling us that people’s political affiliation is mostly driving them to get the vaccine,” he said. “I think if political leaders would step up and be the example, I think that would make all the difference.”