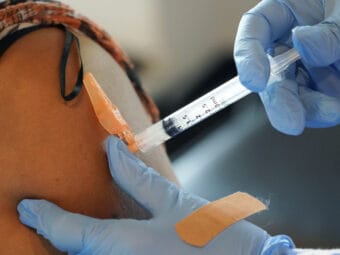
Federal funding to test uninsured people for COVID-19 ran out on March 22. Soon after, the testing sites run by Fairweather in Anchorage started turning away people without insurance.
Jessica Haley, who administers tests at the Fairweather drive-through site on Lake Otis Parkway, said that’s been tough.
“I just refer them to the at-home testing kits,” she said. “And a lot of employers aren’t accepting those because they want the PCR tests.”
Haley’s testing site is one of two in Anchorage run by Fairweather. Jyll Green is their medical services manager. She said that before they stopped testing uninsured patients a few weeks ago, about 40% of people getting tested at their sites were uninsured. And they haven’t just been Alaskans.
“We are getting a lot of tourists from all over the world, maybe not insured, wanting to get tested because they flew and now they have symptoms,” she said. “Or they traveled and they need to get home, but they don’t have insurance.”
What’s happening at Fairweather is part of a larger trend — the public testing and treatment options that have become staples in the last two years are shifting to the private health care industry.
“I think the whole name of the game is that we’re going to start privatizing COVID,” Green said.
Capstone has operated three COVID testing sites in Anchorage and others in Eagle River, Wasilla, Kenai, North Pole, Ketchikan and Juneau — but not for much longer. All Capstone sites will close on June 30.
Matt Jones is Capstone’s director of non-clinical operations. He said keeping drive-up testing sites open is no longer financially viable.
Capstone kept testing uninsured people after March 22. Billing insurance for other patients has allowed them to make up the cost. But now that demand for testing is down, that strategy doesn’t work, Jones said.
“Since that program has ended, and the volume of testing is dropping off significantly — we went from 3,000 tests a day to 200 tests a day — it became financially unsustainable for us,” he said.
Earlier this month, state health commissioner Adam Crum announced that the state’s public health emergency order would end on July 1, but Jones said that wasn’t a factor in the decision to close the sites.
Alaska’s chief medical officer, Dr. Anne Zink, said the public health emergency has no effect on drive-up testing sites or the state’s contracts with the companies running them. Instead, she said, federal funding has started to go away.
“We’ve been planning for the fact that those funds have been going away, and so some of those contracts are scheduled to end as that funding dries up,” Zink said.
In Anchorage, Capstone contracted with the state to run the Alaska Airlines Center testing site at the University of Alaska Anchorage. The site will close with the rest of the Capstone sites on June 30.
Zink said the drop in federal funding is also privatizing treatment options. In Anchorage, Fairweather has a state contract to run a monoclonal antibody infusion clinic at Tikahtnu Commons. That contract also ends on June 30. Green said Fairweather is looking to partner with other groups, like Southcentral Foundation, to continue providing monoclonal antibody infusions.
Zink said federal funding for monoclonal antibody treatments is expected to end in fall. Oral antivirals like Paxlovid are widely available, but they require a prescription.
“As we transition back into the traditional, private health care marketplace, we really encourage people to make sure they have a primary care provider, make sure they have access to testing,” she said. “The federal government continues to have antigen testing that they will send to you. Many health insurance will actually send you antigen testing as well.”
Zink said the state health department will work with private health care providers to keep resources like their testing site locator updated.
People with insurance could notice further changes if the federal emergency order ends. It currently expires on July 15, but officials expect to extend it to October.
If the federal order ends, people with Medicare, Medicaid and private insurance could face out-of-pocket costs for testing and certain treatments. The number of Alaskans covered by DenaliCare — the state’s Medicaid program — increased during the pandemic to nearly one in three residents.