
EHR, ICD-10 and PQRS may sound like alphabet soup to you. But most doctors around the country know exactly what those acronyms stand for. They are programs championed by the federal government to improve quality and bring medicine into the electronic age. But in Alaska, where small medical practices are the norm, the new requirements can be a heavy burden.
Dr. Oliver Korshin doesn’t want to use electronic records in his office. Starting next year, the federal government will penalize him for that choice- withholding 1 percent of his Medicare payments. So in February, the 71 year old ophthalmologist mailed in a form, requesting an exemption. He had to indicate which exemption category fit his situation:
“The only one that possibly applied to me was disaster. So I picked disaster and I described my disaster as old age and I submitted as my supporting document a copy of my passport.”
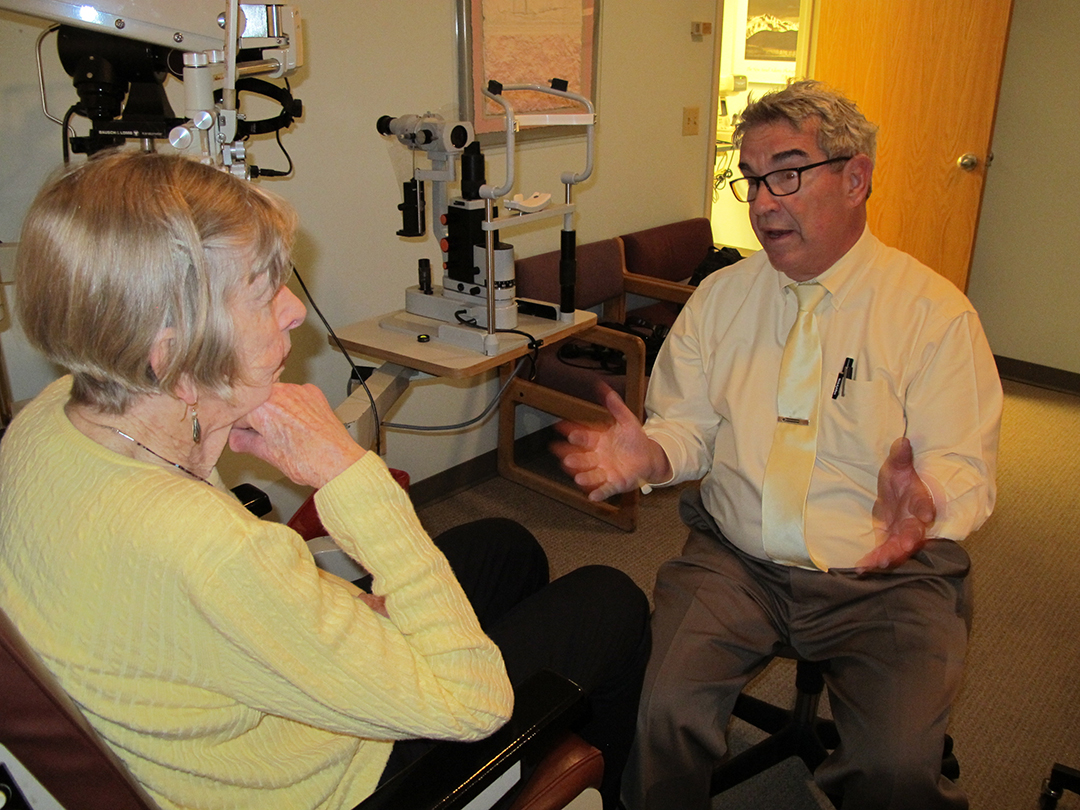
Korshin practices three days a week in the same small office in east Anchorage he’s had for three decades. Many of his patients have aged into their Medicare years right along with him, like the 86-year-old woman visiting on a recent afternoon for a regular check up.
Korshin has just one employee, a part time nurse. And his lease runs out in four years, when he will be 75 and expects to retire. He says for his tiny practice, electronic medical records just don’t make sense. It would cost too much to make the switch and maintain a new system.
“No possible business model would endorse that kind of implementation in a practice situated like mine, it’s crazy.”
Korshin will lose another 1.5% of his Medicare payments next year for failing to enroll in PQRS, a federal program that requires doctors to report quality data. And then there is ICD-10, a new coding system- also set to take effect the fall of 2015. Korshin says small practices can’t keep up with all of the federal requirements:
“This flurry of things one has to comply with means that unless you work for a large organization like a hospital that can devote staff and time to dealing with these issues, there’s no economy of scale, I can’t share these expenses with anybody.”
Korshin may seem like an outlier, being so close to retirement with such a small practice. But according to the Alaska State Medical Association, he is not alone. The association’s Mike Haugen says half of the doctors in Alaska are over the age of 50 and very few are employed by large organizations:
“Most practices in Alaska are small practices. They’re 1, 2 and 3 doctor practices. The number of really large practices- and that’s relative in Alaska- you can probably count them on one hand.”
Haugen says he hears a lot of complaints from doctors who are feeling overwhelmed by the federal requirements for practicing medicine. And he worries the burden is forcing many- especially older doctors, to consider retiring early:
“There won’t be some flashing neon sign we ever see that says x number of doctors have left. It’s a very quiet process and that for me is the scary part, because you take a look at the medical association membership a year or two from now, and it may be smaller and access to care in this state is a real issue.”
But Rebecca Madison thinks a lot of doctors would decide to stay in practice if they had help with the transition to electronic health records. That’s Madison’s job as executive director of Alaska eHealth Network. She wants to make it as easy as possible for providers to make the switch to electronic records. And she encounters a lot of resistance.
“We hear everything from it will never work for them, it’s too costly for them- especially for some of the older providers in this state who are coming to the end of the time in their practice. It’s a huge investment.”
Madison tries to sell doctors on the benefits. She reminds them electronic records can make their offices more efficient and give them better data on the care they’re providing. And it will make it easier when it comes time to sell their practices. Madison also sees the issue from the patients’ perspective:
“My whole goal and the reason I got into this… process is to give the data to the patient. They deserve to have it- it’s their data- they should be able to access it.”
But Madison says she understands electronic records won’t work for every doctor and she thinks that’s okay. Remember Oliver Korshin and his letter asking the federal government for an exemption from the electronic records requirement due to old age? He got a response- through Senator Murkowski- in May.
It was denied.
Korshin says he will continue practicing anyway- the old fashioned way.
This story is part of a reporting partnership between APRN, NPR and Kaiser Health News.
